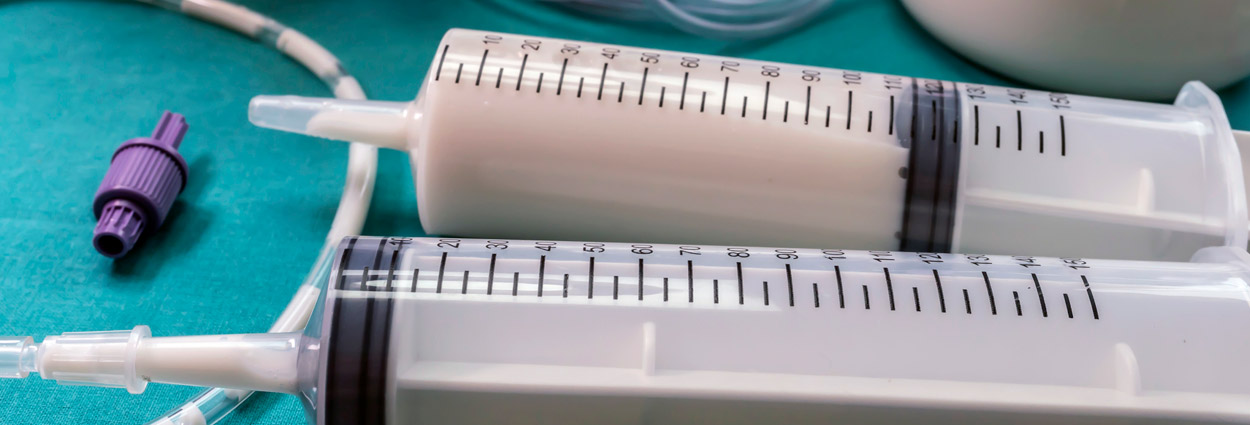
Individuals who are ill or unable to eat for various reasons — decreased appetite, difficulty swallowing, or surgery that interferes with eating — may need enteral therapy, which is also referred to as “enteral nutrition” or “tube feeding.” Enteral therapy involves sending a mixture of protein, carbohydrates, fats, vitamins, and minerals through a tube into the stomach or small intestine.
Who Receives Enteral Therapy?
Enteral therapy may be provided to individuals of all ages. It may be given to infants, children, teens, adults, and seniors. Individuals who aren’t able to eat enough to meet their nutritional needs or whose caloric requirements have increased beyond their ability to eat may need enteral therapy.
The risks of being unable to eat properly or adequately include malnourishment, weight loss, and other serious health issues. A few conditions that may require enteral therapy include:
- Stroke, which may impair a patient’s ability to swallow
- Cancer, which may cause fatigue, nausea, and vomiting
- Critical illness or injury that decreases energy or impacts the ability to eat
- Illness that makes it difficult for the body to absorb nutrients from food
- Neurological or movement disorders that increase caloric requirements while impairing the ability to eat
Enteral therapy may be provided for as long as necessary, though typically it is used for a short time and the tube is removed once the person is able to eat by mouth. Patients may rely solely on enteral therapy to receive their daily nutrition, or it may be used as a supplement to eating by mouth.
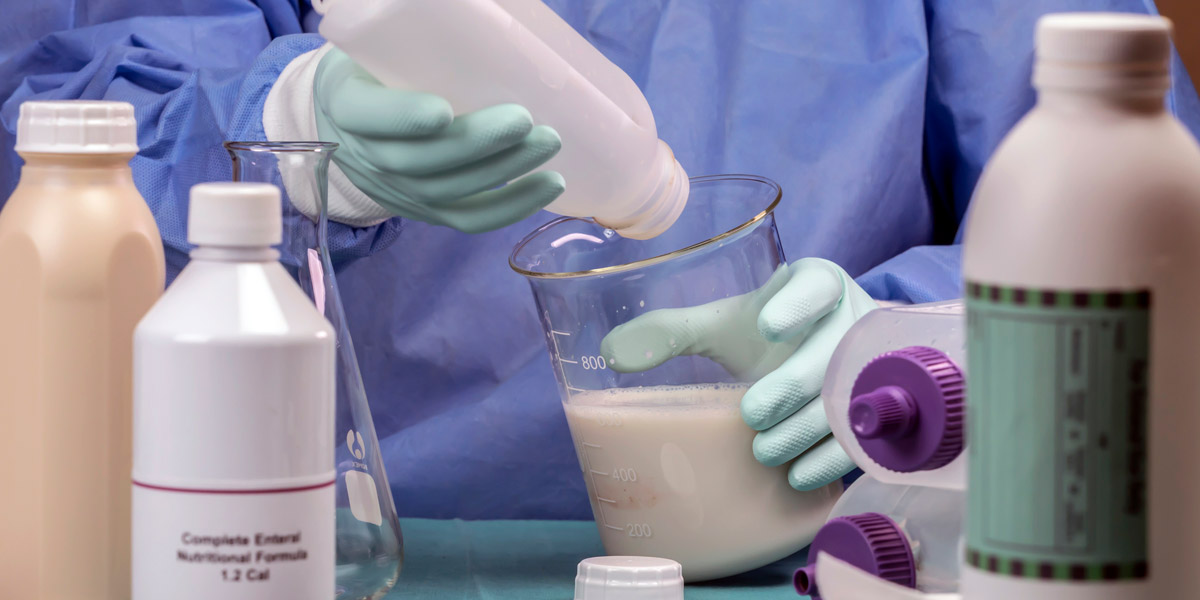
How Is Enteral Therapy Supplied?
Enteral therapy is administered through different types of tubing methods. The six different types of feeding tube options are:
Nasogastric tube (NGT). Placed through the nose into the stomach.
Nasoenteric tube. Placed in the nose and travels to the intestines.
Jejunostomy tube. Placed through the skin of the abdomen straight into the intestines.
Gastrostomy tube. Placed through the skin of the abdomen straight into the stomach.
Oroenteric tube. Placed in the mouth and travels to the small intestine.
Orogastric tube (OGT). Placed in the mouth and travels to the stomach.
The patient’s healthcare team (doctors, nurses, dietitians, and pharmacists) will determine which type of feeding tube is best for their unique condition.
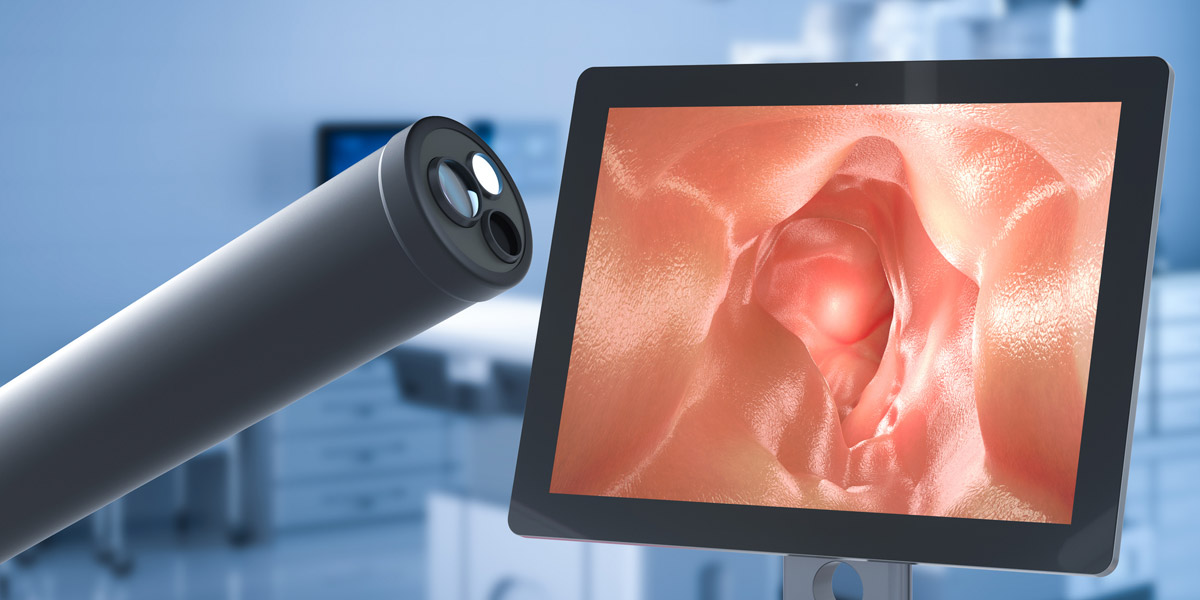
How NGT and OGT is Placed
A nurse will measure the length of the tube, lubricate the tip, and place the tube in the nose or mouth. The tube will then be advanced until it is in the stomach. Using a syringe, the nurse will extract some gastric juice from the tube to check the pH, or acidity, of the liquid to confirm the tube tip is located in the stomach. Some patients may require a chest X-ray to confirm placement.
Anesthesia isn’t required since the procedure is quick and painless, though uncomfortable.
How Nasoenteric and Oroenteric Tubing is Placed
This type of enteral therapy requires using an endoscope to ensure proper placement. The procedure may be done with or without conscious sedation.
How Gastrostomy or Jejunostomy is Performed
The procedure may require conscious sedation or general anesthesia. An endoscope will be used to visualize where the tube will be inserted and a tiny cut will be made in the abdomen to feed the tube into the stomach or intestines.